This is the first of three posts that will cover three important books about how the science of mind, brain and mental health, interfaces with society at large.
This is the first of three posts that will cover three important books about how the science of mind, brain and mental health, interfaces with society at large.
First off, I want to discuss an excellent book called Neuro: The New Brain Sciences and the Management of the Mind published this year by sociologists of neuroscience Nikolas Rose and Joelle M. Abi-Rached.
You may be wondering why we need a social study of neuroscience but it becomes clear when we think of how neuroscience has become important.
It is not just due to what has been discovered. Neuroscience research itself, is only driven in part by scientific discovery.
In the main part, it is driven by a complex mix of politics, business, health care needs and public popularity. That’s what provides the funds and makes the scientific discovery possible and this only moderately, some would say weakly, relates to how far we ‘advance’ in terms of learning.
There is also a common idea that discoveries from psychology and neuroscience form the basis of interventions or changes to society, but much of the time, discoveries from psychology and neuroscience are co-opted to justify changes based on social values.
Here’s a really good example from p196 from the chapter on ‘The Antisocial Brain’ that discusses how the neuroscience of plasticity, the adolescent brain and child psychopathology has been used to justify family interventions.
By way of the brain, then, we reach a conclusion that does not differ greatly from arguments reaching back to the late nineteenth century about the effects of the early years on later propensities to problematic conduct.
From Mary Carpenter’s campaigns for colonies for dangerous and perishing children, through the social problem group and “the submerged ten percent” in the early twentieth century, via the mental hygiene movement in the 1930s, and arguments for setting up child welfare services in the years after the Second World War, to the contentious concept of the “cycle of deprivation” in the 1970s, and the interventions of the Head Start program to the Sure Start program – we find repeated arguments that one should minimize a host of social ills, including criminal and antisocial conduct, by governing the child through the family.
In each generation, unsurprisingly, these arguments are made on the basis of whatever happens to be the current mode of objectivity about the development of children – habits, the will, instinct theory, psychoanalysis, and today the brain.
Each time, the scientific programme is received as if it is a new approach to the problem of child deprivation and delinquency, when the success of these programmes lies precisely in the fact that they are largely the same. In this case, based on the idea that the family is the primary point of responsibility and intervention for poor adolescent behaviour.
Similarly, the success of neuroscientific approaches to problems often depends on how acceptable the implications would seem to potential funders because the money has usually to be agreed before significant lines of inquiry can be started.
This is why non-medical behavioural genetics research gets such a hard time. It’s not that it’s necessarily worse science in terms of its empirical methods but it reminds people of unsavoury practices like eugenics that run counter to prevailing values.
Neuro tracks exactly these sorts of interactions through history and between prevailing current interests. It is also brilliant technically, however, and you will actually learn a great deal about neuroscience methods from the book.
From the history and development of brain scanning techniques, to psychiatric drugs, to the rhetorical role of animal models in understanding mental illness, to how our notion of ourselves is changing in light of advances in brain sciences – it’s remarkably wide in scope.
Sociology is famous for its gobbledebook jargon, and this book has none of this, but its only drawback is that it is, in the end, an academic book and is sometimes written without much thought for the general reader.
But if you can tolerate the academic language, it is essential reading. If you want to understand neuroscience – rather than just facts about neuroscience – Neuro is probably one of the most important books you could read.
And the same goes if you are a neuroscientist or just interested in how we, as a society, are integrating the study of the brain into how we live.
Next in this three-part Mind Hacks series on science and society – Ben Goldacre’s Bad Pharma.
Link to more details about Neuro.
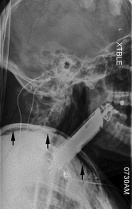 A man with drug-induced psychosis attempted to swallow his smartphone and the case was reported in the medical journal Internal and Emergency Medicine.
A man with drug-induced psychosis attempted to swallow his smartphone and the case was reported in the medical journal Internal and Emergency Medicine. New York Magazine has an excellent
New York Magazine has an excellent 

 Ben Goldacre might be quite surprised to hear he’s written a sociology book, but for the second in our series on books about how the science of mind, brain and mental health meet society,
Ben Goldacre might be quite surprised to hear he’s written a sociology book, but for the second in our series on books about how the science of mind, brain and mental health meet society, 
 AddictionBlog has an amazing
AddictionBlog has an amazing  This is the first of three posts that will cover three important books about how the science of mind, brain and mental health, interfaces with society at large.
This is the first of three posts that will cover three important books about how the science of mind, brain and mental health, interfaces with society at large. If you only read one psychology article in the next few months, make it the startling and unsettling Atlantic
If you only read one psychology article in the next few months, make it the startling and unsettling Atlantic  A series of ‘bizarre delusions’ from patients diagnosed with schizophrenia described in a new
A series of ‘bizarre delusions’ from patients diagnosed with schizophrenia described in a new