Phrenology was the practice of reading someone’s personality from the bumps on their head based on the idea that the shape of the brain affected the shape of the skull.
Contemporary neuroscience lectures often have a part where the professor puts up an image of a phrenology head and says “although this was a rediculous concept, it sparked the idea that the brain could have parts that were specialised for particular functions”.
Phrenologists are usually considered to be quacks and that serious neuroscientists ‘took over’ from where they left off, but I’ve found lots of old copies of The Phrenological Magazine in the Institute of Psychiatry library and it turns out they had a keen interest in serious neuroscience.
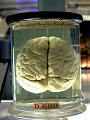
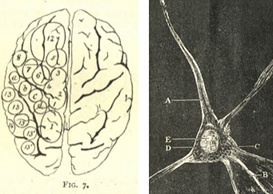 The images on the right are from the June 1890 edition (the brain) and October 1895 edition (the neuron) and both show some of the then cutting-edge neuroscience that the magazine regularly featured.
The images on the right are from the June 1890 edition (the brain) and October 1895 edition (the neuron) and both show some of the then cutting-edge neuroscience that the magazine regularly featured.
The brain is from the work of legendary neurologist David Ferrier showing his map of cortical functions transposed from his work on open-brain stimulation on animals.
The second image shows the structure of the neuron. The text describes how “molecular movements generated within any individual cell can probably be transmitted to other cells in the same striatum in the cortex” and the feature article goes on to highlight the latest discoveries in neuronal function.
It’s worth saying that this detailed discussion of neuroscience with accurate neuroanatomical images is far more common in the magazine than phrenological brain maps. It seems serious medical men wrote some of the articles and neuroscience debates are common in the pages.
The magazine is not without a bit of kookiness, however, although it’s hard to judge how much of this was considered kooky at the time.
My favourite part is where every issue has a portrait of a famous person with an interpretation of their character underneath. This is the interpretation from the portrait of Lord Wolseley, new head of the British Army, from October 1985.
The head of the new Commander-in-Chief indicates a fair balance of all the powers of his mind. He has no superabundance in any particular to give bias, no special deficiency to cause eccentricity. His head is well formed and appears to be well-developed in all parts.
Inside one issue I found an insert that just said “WANTED TO PURCHASE: a Tatoo’ed New Zealander’s Head. – Apply to Major-General H. ROBLEY, 7 St Alban’s Place, Haymarket”. It turns out that Robley was a renowned collector of such things and it seems phrenologists were one of his sources.
In fact, the magazines are full of wonderful adverts. This list of ‘penny lectures’ isn’t that different from pop psychology and neuroscience today.

There’s some good names for a band lurking in there.

 Nobel-prize winning neuroscientist
Nobel-prize winning neuroscientist  The research on the psychological impact of video games tells quite a different story from the stories we get from interest groups and the media. I look at what we know in an
The research on the psychological impact of video games tells quite a different story from the stories we get from interest groups and the media. I look at what we know in an 


 The Global Mail has an amazing
The Global Mail has an amazing 

 Being Human has an excellent
Being Human has an excellent  BBC Radio 4 has just broadcast a documentary entitled ‘Hallucination – Through the Doors of Perception’ that charts the various ways in which we can experience freewheeling and autonomous perceptions.
BBC Radio 4 has just broadcast a documentary entitled ‘Hallucination – Through the Doors of Perception’ that charts the various ways in which we can experience freewheeling and autonomous perceptions. It’s not often you see someone licking a brain in a rock n’ roll video and get to think to yourself “well, there’s a funny story behind that”, but this is one of those occasions.
It’s not often you see someone licking a brain in a rock n’ roll video and get to think to yourself “well, there’s a funny story behind that”, but this is one of those occasions. The Lancet has just a launched a
The Lancet has just a launched a 